
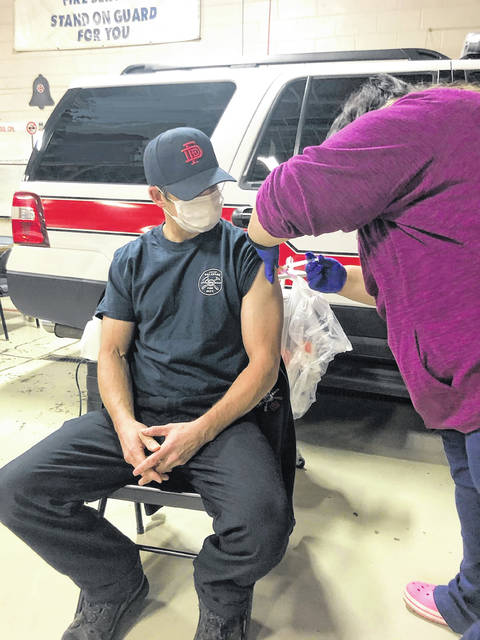

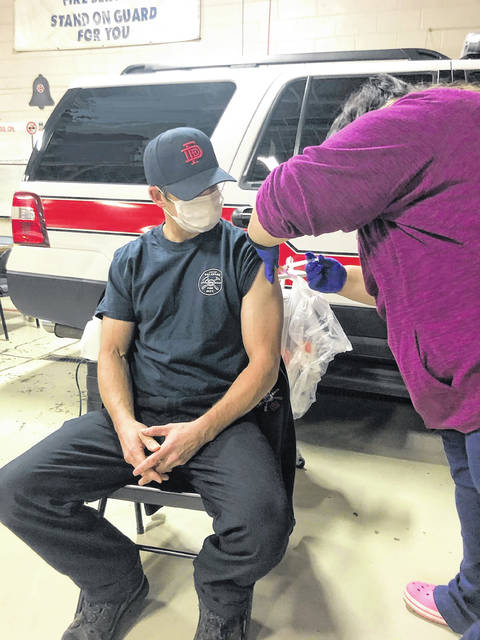
The introduction of two new vaccines to prevent COVID-19 has humanity breathing a collective sigh of relief, but many people rightly still have questions about them. How do they work? How were they developed so quickly? And why do we need them?
The publication The Hill said there were at least 3,903 COVID-19 related deaths in the United States on Wednesday, citing The Atlantic’s COVID Tracking Project as its source. On Tuesday, 3,725 deaths were reported. Those numbers both exceed the terrorist attacks on Sept. 11, 2001, which claimed the lives of 2,977 Americans.
In 2020, there were 340,000 Americans who died from COVID-19 (coronavirus), an infectious disease first identified in late 2019 in China. More than 19 million Americans have contracted the respiratory illness. The global pandemic has infected more than 82 million people worldwide, with more than 1.7 million deaths. Cases have been recorded even in remote Antarctica. Researchers say SARS-CoV-2, the virus that causes COVID-19, kills 2.2% of the people who get it.
“This pandemic could end if the virus swept through the population killing millions but leaving the survivors with natural immunity,” writes physician scientist David Pride in The Conversation. “More likely, the virus will snuff itself out when most of the population has been vaccinated with a SARS-CoV-2 vaccine.”
However, vaccines are slow to be developed, taking at least a decade on average. Pride said the fastest vaccine ever developed was for the mumps and took four years.
A vaccine wouldn’t be ready until 2036, an Ohio Wesleyan University virologist said last year during a virtual class offered to the public. This prognostication assumed you were starting from scratch. Another prediction, based on what is known about the first outbreak of SARS in 2002, said a traditional vaccine could be ready in 2028.
However, genetic vaccines engineered using messenger RNA are quicker to produce and proved surprisingly effective in trials in 2020, leading to their immediate production.
The Centers for Disease Control and Prevention said the Pfizer, Inc. and BioNTech mRNA vaccine (called BNT162b2) requires two shots given 21 days apart in the muscle of the upper arm. The other mRNA vaccine (called mRNA-1273) is made by ModernaTX, Inc. and requires two shots given 28 days apart in the muscle of the upper arm. Neither vaccine contains eggs, latex or preservatives.
On Dec. 14, the vaccine reached The Ohio State University Wexner Medical Center, and the name medical workers there gave it was “Hope.”
The vaccine contains messenger RNA (ribonucleic acid) made with the genetic code of spike proteins. Spike proteins are in the strain of coronavirus that cause COVID-19.
“When you’re injected with the vaccine, this messenger RNA enters your cells and produces a protein to stimulate an immune response,” the Wexner Center states in a recent article. “Now if you encounter the real virus, your body will recognize COVID-19 and is trained to fight it.”
“Many vaccines trigger an immune response by putting a weakened or inactivated germ into our bodies,” said the Delaware Public Health District in a recent post on Facebook. “mRNA vaccines do not work this way. In addition, mRNA vaccines are easy to make in a lab, so they can be developed quicker than other vaccines; can’t cause infection and is broken down by normal processes in our cells; and are not new — they have been under research and development for years for other viruses.”
The CDC said mRNA vaccines cannot give someone COVID-19, nor do they affect or interact with a person’s DNA (genetic material), since it never enters the nucleus of the cell.
For more information on the pandemic, visit DelawareHealth.org/Covid-19, coronavirus.ohio.gov or cdc.gov/coronavirus, or www.who.int/emergencies/diseases/novel-coronavirus-2019. The DGHD’s 24/7 emergency line is 740-815-6518, and the ODH call center is 1-833-4ASK-ODH.



